As many as 20 percent of HIV-positive people have left SF in the past five years. Is the housing crisis skewing the numbers?

By Marke B.
JULY 13, 2015 — Last month the San Francisco Department of Public Health, in association with HIV prevention consortium Getting to Zero, announced astonishing all-time record lows in HIV diagnoses and deaths in 2014 (PDF) — down 17% from the previous year.
The general trend in new HIV infections and deaths has been downward since HIV combination drug therapy was introduced in the late 1990s, and a more aggressive campaign to administer anti-retroviral therapy (ART) immediately at diagnosis was instituted in 2010. Both of these therapies have had enormous success in transforming HIV, for many, into a manageable chronic disease instead of a deadly one, and, crucially, suppressing the disease in infected individuals enough to radically decrease the chances of transmission.
But 2014’s reported decline is still major — from 371 new diagnoses and 209 deaths in 2013 to 302 new diagnoses and 177 deaths last year, according to the department.
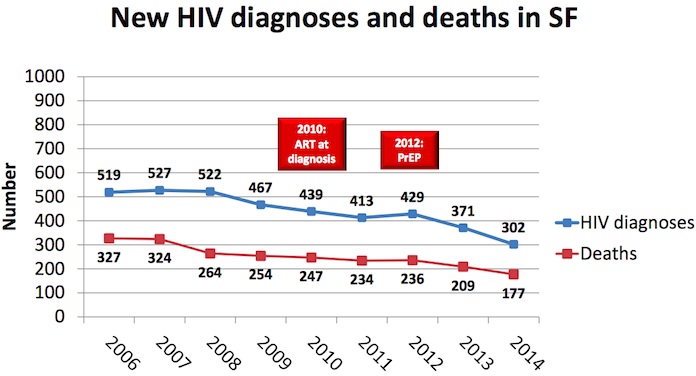
For a city in which almost 16,000 people are living with HIV, those numbers are encouragingly low. Some have been quick to attribute the decline, especially in new diagnoses, to PrEP — Pre-Exposure Prophylaxis, i.e. giving HIV-treatment drug Truvada to HIV-negative people at risk, as a preventative measure to be used in combination with safer sex techniques.
But barriers still remain to further reduction, especially in terms of equal access and treatment: As Dr. Susan Buchbinder, director of SFDPH’s HIV prevention unit, pointed out to the Examiner, HIV-positive black people have a lower survival rate than other ethnicities, and vulnerable populations like the poor or homeless have a tougher time entering and staying in treatment. There has also been an increase in new transmissions among youths, specifically young men of color.
And then there’s the question of displacement — in the past five years, an estimated 15-20% of the HIV-positive population has been affected by evictions, priced out, or simply moved. Could that be skewing the numbers?
And could high housing costs in a city that offers world-class HIV treatment be keeping people away from the health care they need?
In response to the latest report, Brian Basinger of SF’s AIDS Housing Alliance sent me a statement:
We all applaud the news that new HIV infections have declined in San Francisco. While the discussion has primarily focused on the probability that PrEP has been a significant contributor to the decline in new HIV infections, there has been little conversation on the drivers of the 17% decline in HIV deaths, down to 177 (which is still 4 times higher than the number of homicides in San Francisco last year, at 45).
There has not been the introduction of any radically new and improved therapy to treat those of us already infected with HIV that we can attribute the decrease in deaths to, so we must look for other contributing factors for explanation as to why fewer San Franciscans with HIV are dying.
The reason is displacement. They’re getting kicked out of their homes and dying elsewhere. Out of sight. Out of mind.
People with HIV continue to get kicked out of their homes by speculators and experience homelessness at extremely disproportionate rates. Those who are the most vulnerable to increased mortality — disabled long-term survivors — are getting displaced out of San Francisco. They are not moving to gentrifying Oakland. They are moving to Oklahoma, to Lake County, and to other areas that do not have adequate services to maintain one’s health.
SFDPH’s own available numbers on HIV-positive outmigration (PDF) suggest a possible loss of up to 15% of the population in the past two years, whereas our investigations have revealed a loss of 20.3% in the past five years. One-third of San Francisco’s HIV population has experienced a housing crisis. We need to take those numbers into account.
When I asked her about the numbers, Dr. Buchbinder told me the HIV mortality numbers include all people diagnosed HIV-positive in San Francisco, even if they died somewhere else. (When someone is diagnosed HIV-positive, their case is assigned an ID from the Centers for Disease Control and Prevention that tracks the location of future treatments.)
“The numbers of deaths include everyone diagnosed in SF who died, regardless of where they died,” she wrote me in an email. “We do matches with local death certificates, the State Office of AIDS, National Death Index, and social security death files. We believe our numbers for deaths are very complete, although there can be a lag time in getting the reports into the NDI.”
Yet that still leaves the question of how many people who were diagnosed elsewhere have died. A significant portion of San Francisco’s HIV-positive population moved here after being diagnosed, and may be left out of the total count.
“Imagine someone born and raised in SF who goes away to college,” Basinger wrote to me. “Gets tested in his college town. And then moved back to SF after graduation. It sounds like their death would not be counted in the SF death count.
“It also sounds like none of the people who move to SF (like after they test positive in Alabama), are counted in our death count. Even if they have lived here for 30 years.”
San Francisco offers some of the best and most accessible treatment for HIV-positive people in the world — effective HIV treatment was pioneered here 30 years ago, at SF General’s legendary Ward 86. Despite strides in nationwide medication and treatment, however, you won’t find the kind of care, access, and cultural support you can receive in San Francisco in the places where many of those who can’t afford to stay here now must reside.
“We’re talking about people who live on a fixed disability income of less than $900 a month,” Basinger told me. “An aging generation of early contractors of the disease who are now well into retirement age. And LGBT seniors are among the most vulnerable to evictions.”
Because there has been no official request from the Mayor’s Office or Board of Supervisors, there is no official count of how many HIV people have been evicted or displaced — although, as noted above, SFDPH estimates outmigration at up to 15% in the past two years, and AIDS Housing Alliance estimates it at slightly more than 20% in the past five years.
As the SF Getting to Zero consortium, made up of local prevention agencies and formed with the laudable goal of getting HIV infections and deaths to zero, acknowledges, “Housing remains the biggest single gap. GTZ members have spoken about the critical importance of addressing housing to achieve GTZ goals at Board of Supervisor hearings and at GTZ meetings.”
As for the decrease in new infections, questions remain about that as well. Although HIV continues to affect people from all backgrounds and situations, those most at risk continue to be poor, of color, young, and queer — populations being severely affected by San Francisco’s housing crisis. Are new HIV-positive diagnoses decreasing in part because those most at risk can no longer afford to live here?
“Along with access to treatment and education, stable housing is the most important factor in successfully reducing both HIV transmission and mortality,” Basinger told me. “San Francisco has excellent access through programs like Healthy SF, a very low level of stigma around the disease, and a high level of care and support. Yet you need housing stability to help ensure you adhere to the treatment programs that keep you alive.
“If you’re constantly stressed out about your living situation, or if you’re evicted, those have huge negative effects on your treatment and health. And if you never have access to those things to begin with, or lose access due to prohibitive costs, then you’re basically made invisible.
“Housing for HIV-positive people is one of those rare problems that if you throw money at it, it actually gets solved,” Basinger continued. “Imagine how low these numbers could be if those most affected by HIV could afford to live here.”





